By: Sarah Hogekamp Life/Health Actuarial Associate, L&H Cologne, Genre
It is not yet clear whether 2022 was the warmest or second warmest year for Germany since weather records began. The current record holder is 2018 with an annual mean temperature of 10.5 °C.1 What is indeed clear is that preliminary results indicate at least a tie between both years.

This change in the average annual temperature alone tells us little about climate change per se, as the term doesn’t just stand for the occurrence of heat waves or the increase in the global average temperature. Seasonal and regional changes in rainfall, for example, are also consequences of climate change. In Germany, we had drought years from 2018 to 2020, followed by floodings in 2021, all defined as extreme weather events. Climate change means that the frequency and intensity of these different weather events such as heat, frost, drought and floods are increasing.
These changes have an unequivocal impact on human health and mortality trends – and that has serious implications for insurance products in the life and disability segment.
Health and heatwaves
The heatwaves referenced above were extreme weather events that created dents in health and mortality. In general, extreme heat has several adverse health effects including but not limited to:
- stress to the cardiovascular system, which actively works to regulate the body’s temperature. If the stress becomes too great, dizziness, a sudden drop in blood pressure or heat stroke can occur.
- stress to the renal system, which is sensitive to dehydration. A higher outdoor temperature increases the body’s water consumption. If there is no adjustment in water intake, this can be detrimental to health, especially to the kidneys.
- reduced physical activity to avoid heat stress.
Studies show that in addition to the highest age bands, children, the chronically ill, outdoor workers, pregnant women, and people in socially and economically disadvantaged urban areas are particularly exposed to heat-related health risks.2
Figure 1 shows that during the heat wave in the summer of 2018 in Germany, average deaths increased in all age bands. The relative increase seems to be weakest in the 30‑54 and 55‑64 age groups. In the youngest age band, the high volatility of the results makes interpretation difficult, but there appears to be higher mortality over a longer period of time.
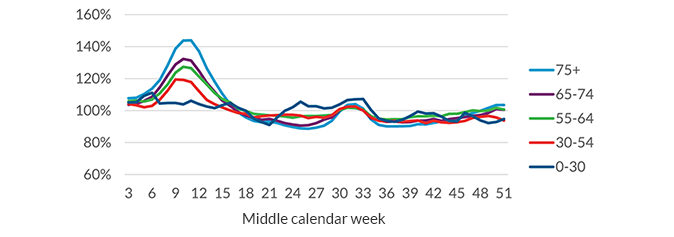
Figure 1: Own plot of four-week moving average deaths per week in 2018 compared to the average of all weeks in 2016‑2019. Data from Federal Statistical Office (Destatis), 2023, “Sterbefälle – Fallzahlen nach Tagen, Wochen, Monaten, Altersgruppen, Geschlecht und Bundesländern für Deutschland, 2016‑2023“ Retrieved January 27, 2023.3
The results of these simple evaluations are consistent with a study from South Africa on relative mortality risk by temperature and age group. An increased risk of death is found not only at higher ages but also particularly strongly among the youngest (the 0 to 4 age group), while in the middle age groups neither heat nor cold – as we know it – has a significant effect on the relative risk of death.4

Is your finely crafted financial plan a grand masterpiece?
Or will it be let down by traditional life insurance products that don’t match your clients’ needs?
As a highly skilled financial adviser, you know that every financial plan is carefully designed to meet your client’s needs today, and as their life changes. BrightRock’s needs-matched life insurance lets you create a product solution that precisely matches the financial plan you’ve crafted for your client.
BrightRock Life Ltd is a licensed financial services provider and life insurer. Company registration no: 1996/014618/06, FSP 11643. Terms and conditions apply
Influenza influence
A logical next step after investigating rising temperatures and the resulting heat mortality, is to also look at the flipside, cold mortality. Can the increased mortality during heat waves be offset by reduced cold mortality? To answer that question we must distinguish between cold mortality and mortality during the cold season.
One major contributor to mortality during the cold season in Germany is influenza. While there is a correlation to cold temperature, it is not exclusive and the overall influenza activity is ultimately determined by many additional factors. Although seasonal influenza occurs in winter in both the northern and southern hemispheres, factors such as seasonal variations in host immune response, changes in influenza strains, and environmental factors such as humidity and UV radiation also influence influenza activity5 and, indirectly, influenza mortality. So even if the winters did become milder with climate change, influenza activity might still be significant.
Figure 2 shows that overall mortality per 1.000 inhabitants in Germany is higher in winter e.g., January, but the correlation between temperature and mortality appears much weaker than it does in summer e.g., August. While the analysis lacks an age-standardization and should therefore be handled with care, it clearly hints towards a stronger relationship between summer and heat deaths as against winter and cold deaths, where influenza activity might play an active role in dispersing the picture.

Figure 2: Own plot of monthly mortality per 1.000 inhabitants by mean monthly temperature in Germany 1990‑2019. Data from Federal Statistical Office (Destatis), 2023, “Sterbefälle je 1000 Einwohner: Deutschland” and the Federal Climate Data Center Germany, 2023, “KU21 – Klimaanalyse (2023) Zeitreihen und Trends von Gebietsmitteln der Parameter Temperatur, Niederschlag, Sonnenscheindauer und verschiedener Kenntage.” Retrieved January 27, 2023.
Inevitable adaptation
This being said, it’s not all bad news. If we look at the optimal temperature with the lowest mortality, we clearly see it varies by region and appears to be particularly higher in warmer regions than in cold ones. Often, the warmer a country is, the higher the optimal temperature, as can be seen with London/UK and Rome/Italy, for example. In addition to temperature, the regions compared differ in their demographics, socioeconomics and other environmental factors, such as precipitation. These observations clearly support the assumption that heat-related excess mortality can be actively mitigated in the future by adjustments to our behavior and environment.

Figure 3: Associations between temperature and mortality in four European cities. Copyright holder: European Environment Agency (EEA). adapted from Gasparrini et al. (2015)
The data clearly shows us that man-made climate change is real and it is increasingly noticeable in Germany. The medical data also clearly shows us that a higher temperature leads to additional stresses on the body – this applies not only to the very old, but to all age groups. It stands to reason that this additional stress results in a potential burden for life insurance companies.
Factors other than the direct effects of heat considered here, such as severe weather or spread of disease vectors, merit a deep dive into the role they play.
On the one hand, the evident complexity calls for further research on this topic, including by actuaries. On the other hand, it is clear that in addition to efforts to limit climate change, adaptations to limit overall risk are urgently required.
End notes
- Deutscher Wetterdienst (DWD), Deutschlandwetter im November 2022, Last Updated: 30.11.2022, https://www.dwd.de/DE/presse/pressemitteilungen/DE/2022/ 20221130_deutschlandwetter_november2022_news.html
- https://climate-adapt.eea.europa.eu/en/observatory/evidence/health-effects/heat-and-health/heat-and-health
- To understand whether heat mortality also affects middle-age bands in Germany, we look at the four-week moving average of deaths per week in 2018 compared with the mean of all weeks from 2016 to 2019. The summer of 2018 was particularly warm in Germany, and 30 or more “hot days” (days with 30 °C or more).
- Scovronick, Noah, et al. “The association between ambient temperature and mortality in South Africa: A time-series analysis.” Environmental research 161 (2018): 229‑235.
- Lowen AC, Mubareka S, Steel J, Palese P (2007) Influenza virus transmission is dependent on relative humidity and temperature. PLoS Pathog 3(10): e151. doi:10.1371/journal.ppat.0030151

